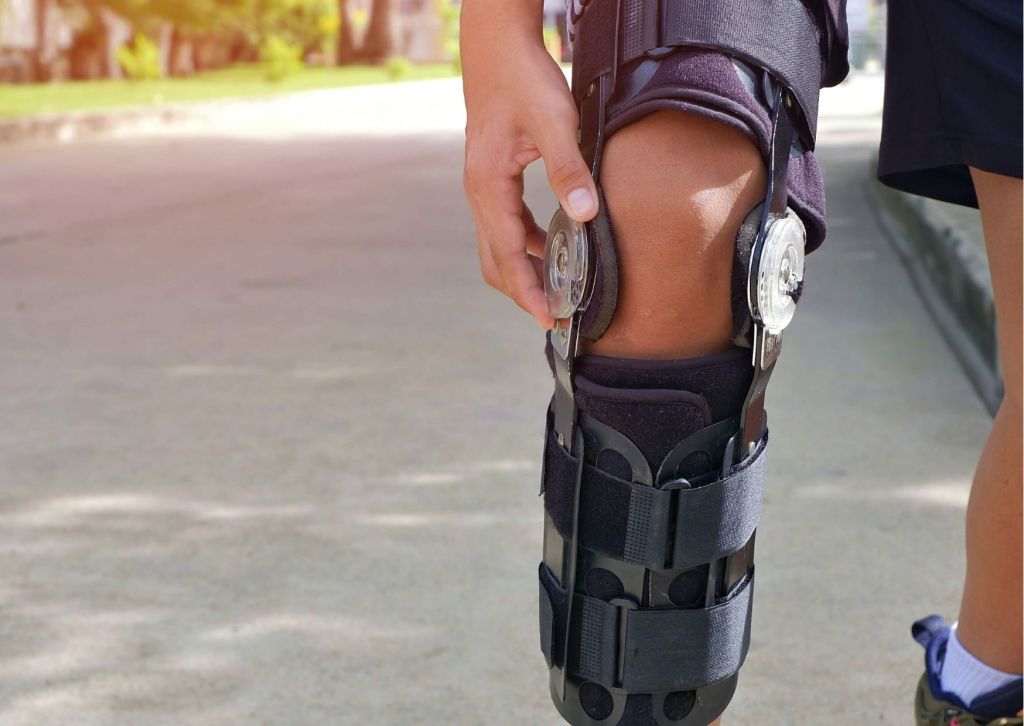
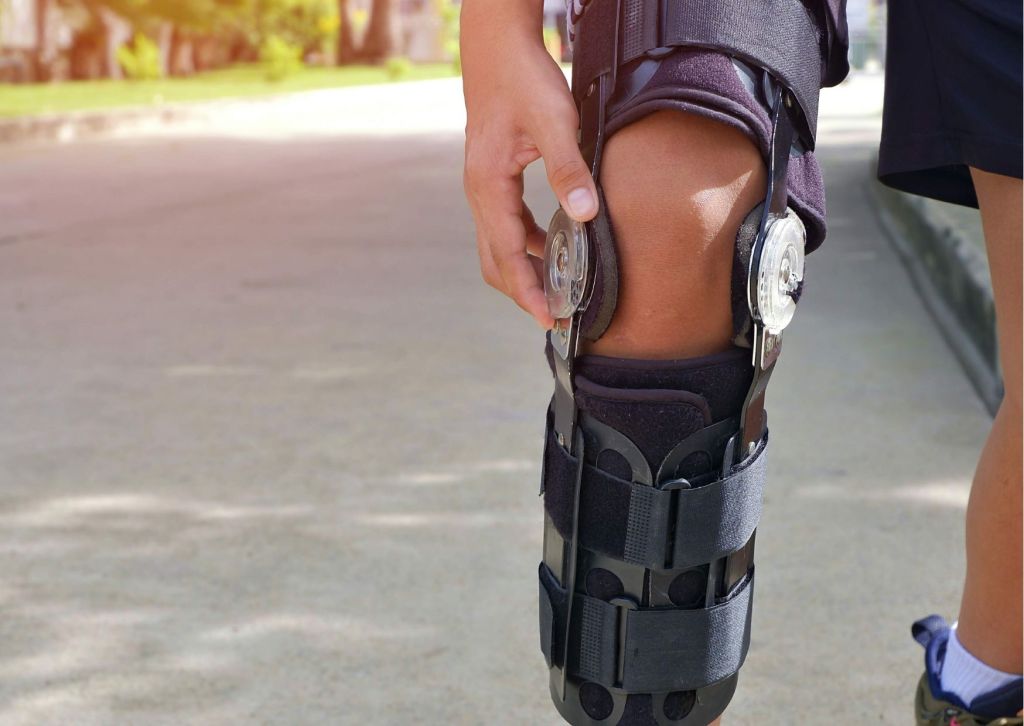
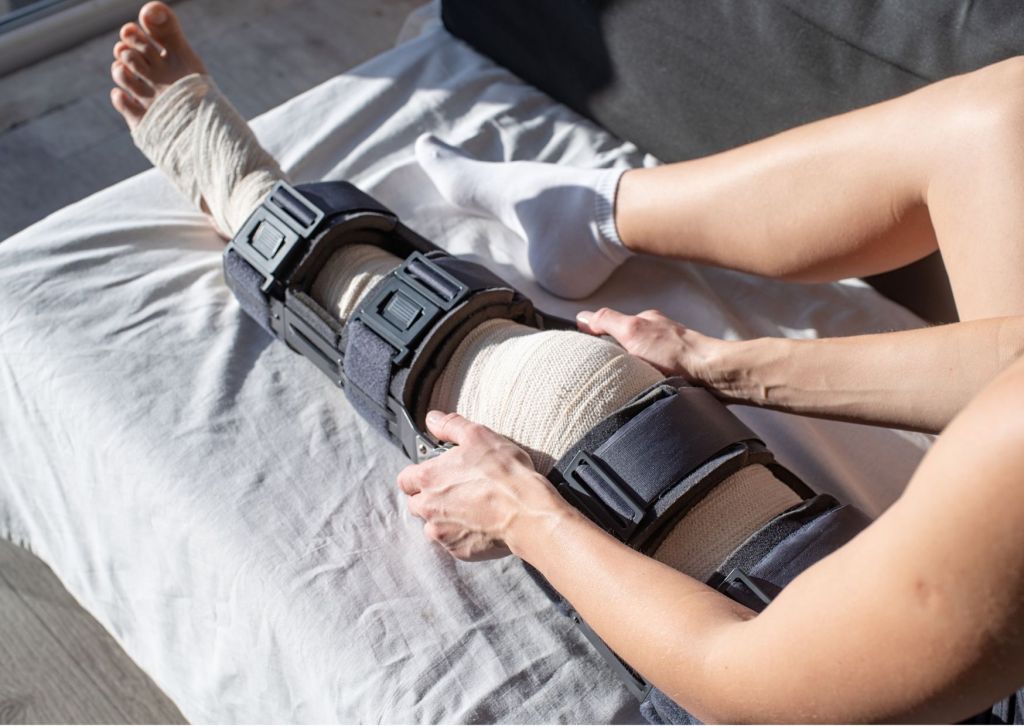
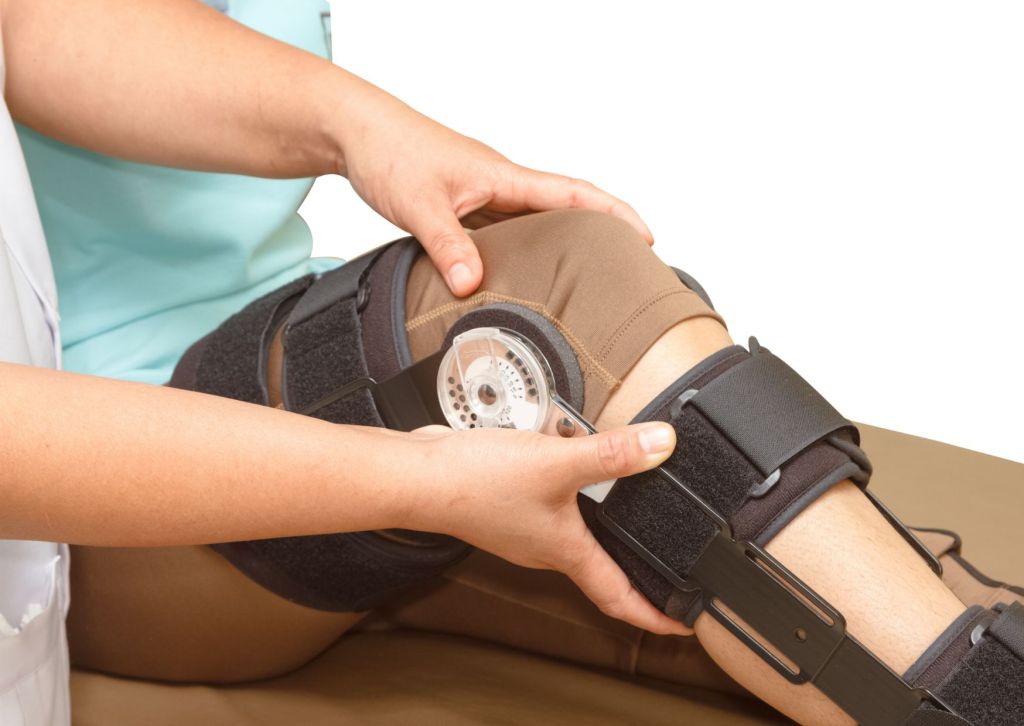
Living with tricompartmental osteoarthritis can be challenging. This form of arthritis affects all three compartments of the knee, often resulting in significant discomfort, stiffness, and reduced mobility. It’s more than just a minor ache—this condition can impact everything from walking and exercising to performing daily routines. Fortunately, for many individuals, a tricompartmental osteoarthritis knee brace can provide meaningful support, reduce pain, and help regain confidence in movement.
Understanding Tricompartmental Osteoarthritis
To understand how a knee brace can help, it’s first essential to understand the condition. Tricompartmental osteoarthritis occurs when the cartilage in all three areas of the knee—medial (inner), lateral (outer), and patellofemoral (front)—begins to wear down. This leads to bone-on-bone contact, swelling, and inflammation. The condition often progresses over time and is most common in older adults, athletes, or individuals with a history of knee injury.
Because all knee compartments are affected, this form of osteoarthritis can be more debilitating than unicompartmental or bicompartmental types of osteoarthritis. The entire joint is compromised, which necessitates more comprehensive support.
How Knee Braces Help
A tricompartmental osteoarthritis knee brace is designed to provide overall support to the knee joint. Unlike braces intended for more localized issues, these braces offer stabilization that helps distribute body weight more evenly across the entire knee. Doing so reduces pressure on the damaged cartilage and bones, helping minimize pain during movement.
Additionally, a good knee brace can improve joint alignment and limit the knee’s range of motion, thereby preventing further wear and tear on the joint. This can be particularly helpful for active individuals who want to remain mobile while managing their symptoms.
Many patients also find that wearing a knee brace gives them a sense of security. It serves as a reminder to avoid sudden, high-impact movements that could lead to further injury.
Choosing the Right Knee Brace
Not all braces are the same, especially when dealing with a condition as complex as tricompartmental osteoarthritis. It’s essential to choose a brace that is specifically designed for this type of joint damage. Some braces include adjustable tension, reinforced hinges, and moisture-wicking material for comfort during extended wear.
Consulting with an orthopedic specialist is highly recommended. They can evaluate your knee’s condition, mobility level, and lifestyle to help you choose a brace that fits your body and daily needs.
Combining Bracing with Other Therapies
While bracing can be vital, it’s most effective when part of a broader treatment plan. Many individuals find relief by combining brace use with physical therapy, anti-inflammatory medications, and lifestyle modifications such as weight management or low-impact exercises. In some cases, injections or surgery may also be discussed as part of long-term care.
Still, for many people, starting with a knee brace offers a noninvasive, low-risk solution that can significantly improve daily function and comfort.
A Step Toward Better Living
Managing tricompartmental osteoarthritis doesn’t have to mean giving up the activities you love. You can take proactive steps toward improving mobility and pain relief with the right approach and tools, including the use of a tricompartmental osteoarthritis knee brace. It’s about making thoughtful decisions to preserve your quality of life, maintain independence, and feel good in your body again.
If you’ve been struggling with chronic knee pain and haven’t yet explored the option of bracing, it may be time to talk to your doctor about what’s available. A well-fitted brace could be the support your knees—and your lifestyle—have been waiting for.