Knee injuries are common across all age groups and can significantly affect mobility and quality of life. Causes include sports, daily wear, and post-surgical recovery. While standard braces provide general support, many patients achieve better outcomes with a custom knee brace tailored to their specific anatomy and activity level.
At our orthopedic clinic, we offer personalized solutions to support healing and improve function. We aim to help patients return to their preferred activities. Advanced knee bracing systems are part of our approach. Understanding the benefits of custom bracing enables patients to make informed care decisions.
Personalized Fit for Better Support
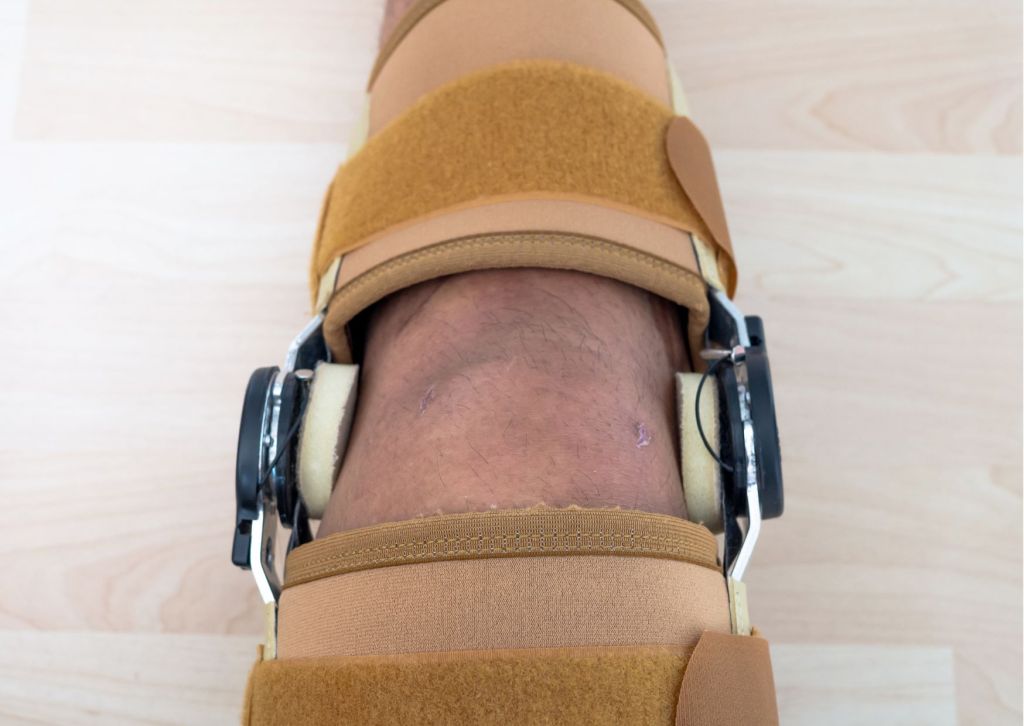
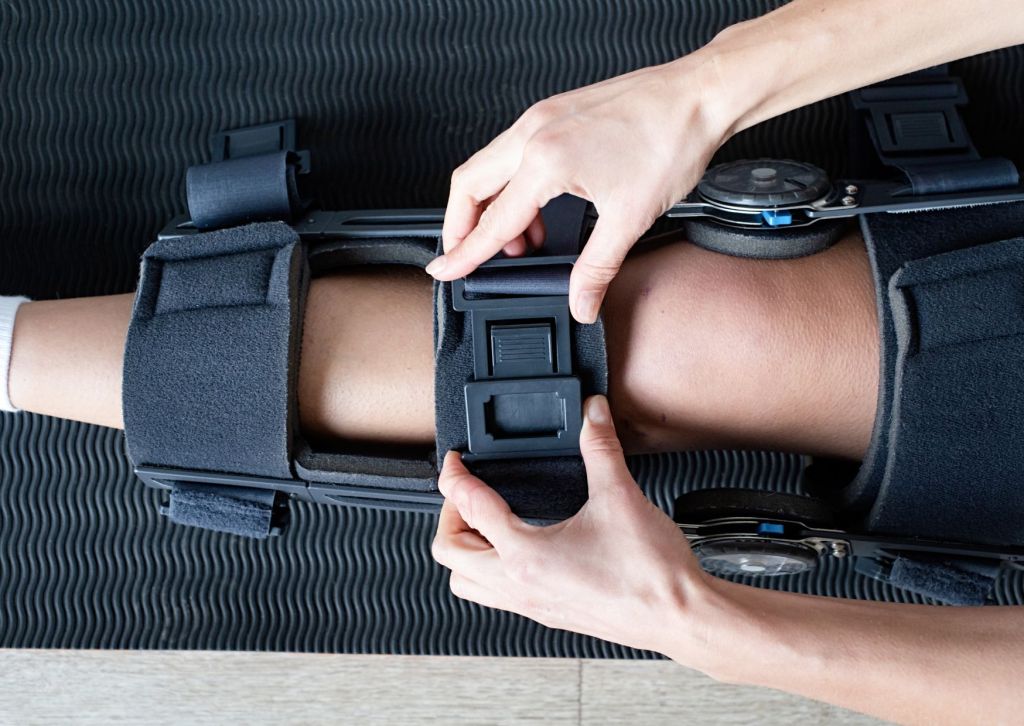
A key advantage of a custom brace is the personalized fit. A primary benefit of a custom brace is its personalized fit. Each brace is measured and fabricated to match the patient’s leg contours, ensuring support is provided where it is most needed. This provides better comfort and prevents skin irritation or pressure points that occur with generic braces. Patients are more likely to wear a brace consistently when it feels secure and comfortable.
A custom CTI knee brace offers targeted ligament support while preserving freedom of movement. This balance of stability and mobility aids both recovery and performance.
Enhanced Stability and Injury Prevention
Stability is a primary goal of knee bracing. For patients recovering from ligament injuries, controlling joint motion protects healing tissues and lowers the risk of reinjury. Custom braces can be designed to limit specific movements that stress vulnerable structures.
Athletes often use custom bracing to return to sports safely. High-demand activities such as soccer, basketball, and skiing place significant force on the knee. A custom knee brace helps manage these forces and increases confidence during movement.
Improved stability also benefits daily activities such as walking on uneven surfaces, climbing stairs, and carrying groceries. Patients often report greater confidence and reduced fear of falling with a well-fitted brace.
Supporting Rehabilitation and Recovery
Rehabilitation after knee injury or surgery requires a structured approach. Physical therapy, strengthening exercises, and activity modification are essential. Bracing complements these efforts by providing external support as the body regains strength.
A custom brace helps maintain proper joint alignment during movement. This promotes natural biomechanics and reduces compensatory patterns that can cause additional strain.
Patients often progress from limited activity to more demanding tasks. Wearing a custom CTI knee brace during this time can reassure them and protect the knee as function improves.
Orthopedic providers collaborate with therapists to ensure bracing strategies align with rehabilitation goals.
Improving Patient Confidence and Quality of Life
Knee instability or chronic pain affects both physical ability and emotional well-being. Patients may avoid activities they once enjoyed due to fear of reinjury or discomfort.
Custom bracing restores patients’ sense of control. Feeling supported makes them more likely to join social, recreational, and work activities. Greater confidence boosts motivation and mental health during recovery.
In practice, we see that patients with personalized bracing use their rehabilitation plans more consistently. They often experience better long-term outcomes.
Professional Assessment and Ongoing Support
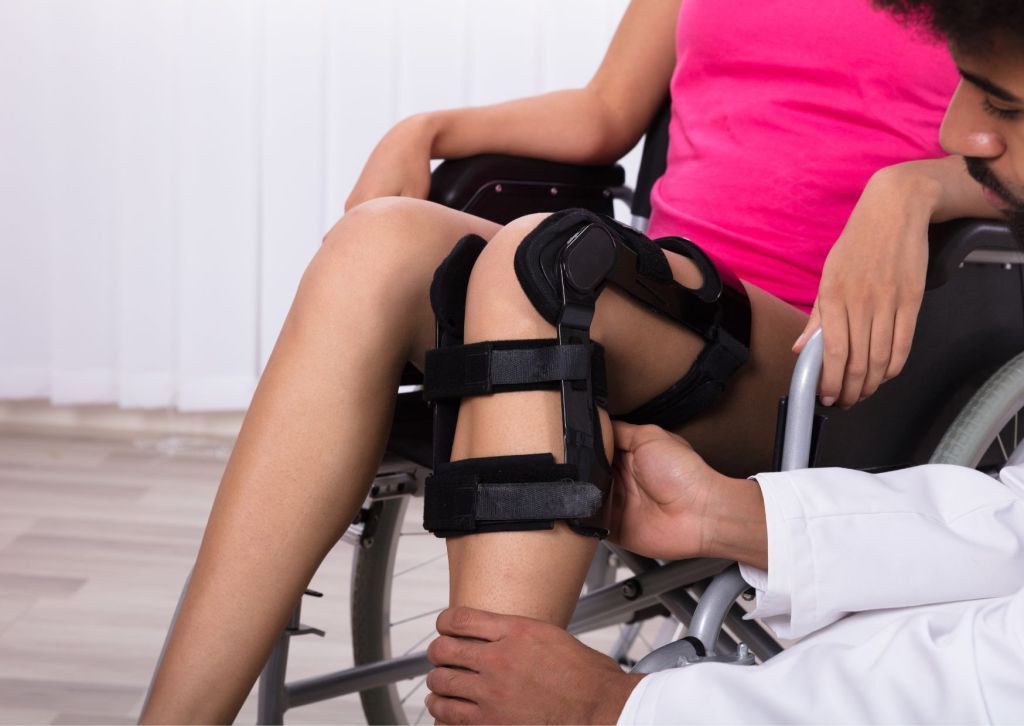
Getting a custom brace takes more than measurements. A thorough orthopedic evaluation determines if bracing is right and which design is most beneficial.
At our clinic, we assess injury history, activity level, gait patterns, and patient goals to ensure the selected brace meets both current needs and future expectations.
Follow-up appointments allow for adjustments and education on proper use. Patients learn to apply the brace, maintain hygiene, and recognize signs that need professional attention.
Ongoing support for custom CTI knee braces ensures patients receive maximum benefit from their investment.
Integrating Bracing With Comprehensive Care
Bracing is one component of orthopedic care. Pain management, strengthening, and healthy habits also contribute to recovery.
Patients should view bracing as a tool that complements medical guidance and rehabilitation. Combining these elements supports better mobility and long-term joint health.
Working with a local orthopedic clinic gives patients access to experienced professionals who can integrate durable medical equipment into individualized treatment plans.
Choosing the right knee brace can significantly improve recovery and daily function. A custom knee brace provides personalized support, enhanced stability, and greater comfort than generic options. For patients with ligament injuries, post-surgical needs, or active lifestyles, devices like the custom CTI knee brace offer targeted solutions for safe movement.